
In a recent article entitled “The Effectiveness of Pelvic Floor Muscle Training in Men After Radical Prostatectomy Measured with the Insert Test,” published in the International Journal of Environmental Research and Public Health in March of 2022, the use of surface EMG biofeedback (sEMG) was one of three cohorts for men with post-operative incontinence. While all participants improved in control over micturition, the cohort of men in the group using sEMG biofeedback had the best results post-treatment./p>
So, what is it about biofeedback that improves control in patients with pelvic floor muscle dysfunction?
Biofeedback provides visual and auditory feedback of muscle activity. It is a non-invasive technique that teaches patients how to adjust muscle function, strength, and behaviors to improve pelvic floor function. The small electrical signal (EMG) provides information about an unconscious process. It is presented visually on a computer screen, giving the patient immediate knowledge of muscle function and enabling the patient to learn how to alter the physiological process through verbal and visual cues.
Kaufman states, “Without full knowledge of the use of the sEMG biofeedback equipment, many providers may miss important components to treatment.” For example, patients may inadvertently hold pelvic muscles in a chronic state of tension in an effort to avoid leakage, reducing the range of muscle excursion available for proper muscle contraction and control. Additionally, poor pelvic floor isolation can compound symptoms of incontinence when larger muscle groups such as the abdominals are co-contracting, reducing the effectiveness of the pelvic floor effort.
Importantly, biofeedback gives the skilled clinician the opportunity to evaluate proper muscle function in all three positions: supine, sitting and standing. According to Lee, “You will typically see the muscle dysfunction in the standing posture, which is not typically assessed in manual treatment.” Furthermore, in supine the muscle may not have dysfunctions and the provider will miss what happens when position is altered, and gravity negatively influences the muscle contraction.
Kaufman adds, “The only true way to determine muscle tone is through the use of sEMG biofeedback.” Manual skills alone may falsely indicate there is no muscle excursion with palpation when, in fact, the use of sEMG biofeedback reveals the presence of high tone in the pelvic muscles at rest. By restoring normal muscle resting tone the patient gains more muscle excursion and is better able to utilize and feel the muscle contract.
Case Study Example
The patient is a 63-year-old computer specialist who underwent radical prostatectomy three years ago due to prostate cancer. He has been relocated for work twice in that time and has seen two pelvic floor therapists during that period who worked exclusively with manual internal and external muscle techniques. Finally, he was referred to a biofeedback board-certified therapist who did a supine, sitting, and standing muscle assessment using two-channel sEMG biofeedback: one channel was for a rectal sensor, and the other monitored the obliques.
The "before" graph is a supine, sitting, and standing assessment. The patient is asked to perform three quick contractions, followed by a 10-second hold in each position. In the supine position, the patient demonstrated good muscle resting tone, endurance, and isolation, but once in sitting, he began to demonstrate poor pelvic floor muscle endurance, poor isolation, and higher resting tone. In standing, his pelvic floor muscle was completely overpowered by his obliques and rectus abdominis, and he had very limited pelvic muscle endurance and poor resting tone. His frustration with lack of bladder control led to withholding fluids (making symptoms worse).
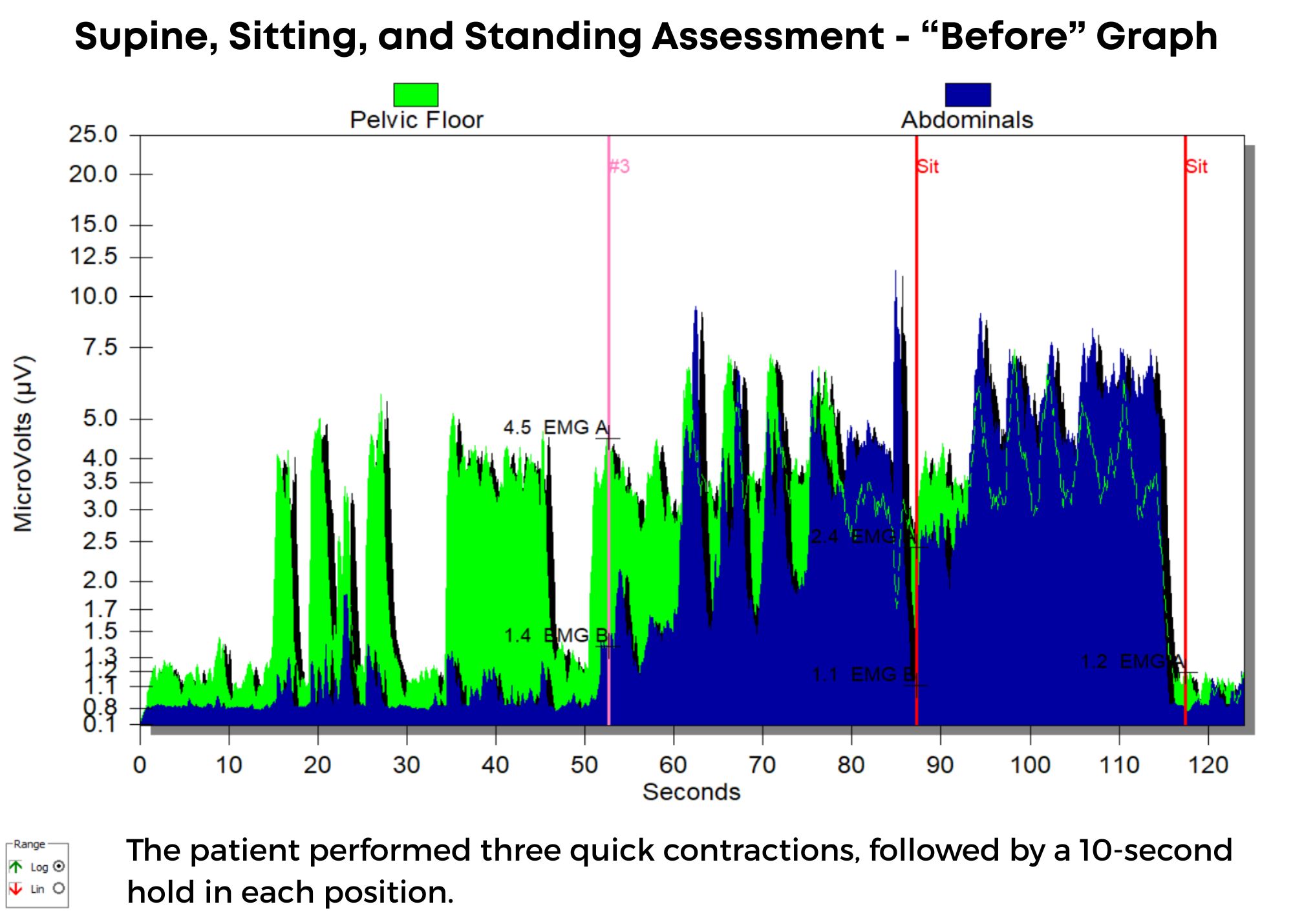
Once the patient was instructed in techniques to restore normal pelvic floor muscle tone and isolated contractions using sEMG biofeedback, he began to note improved control over bladder function, and after eight visits, he was discharged from care, having achieved all treatment goals. In his "after" graph, he exhibited good muscle tone, endurance, and isolation, and did not have his abdominals overpowering his pelvic floor. He also consumed adequate water intake again but without negative effects on bladder control. He no longer needed protective undergarments.
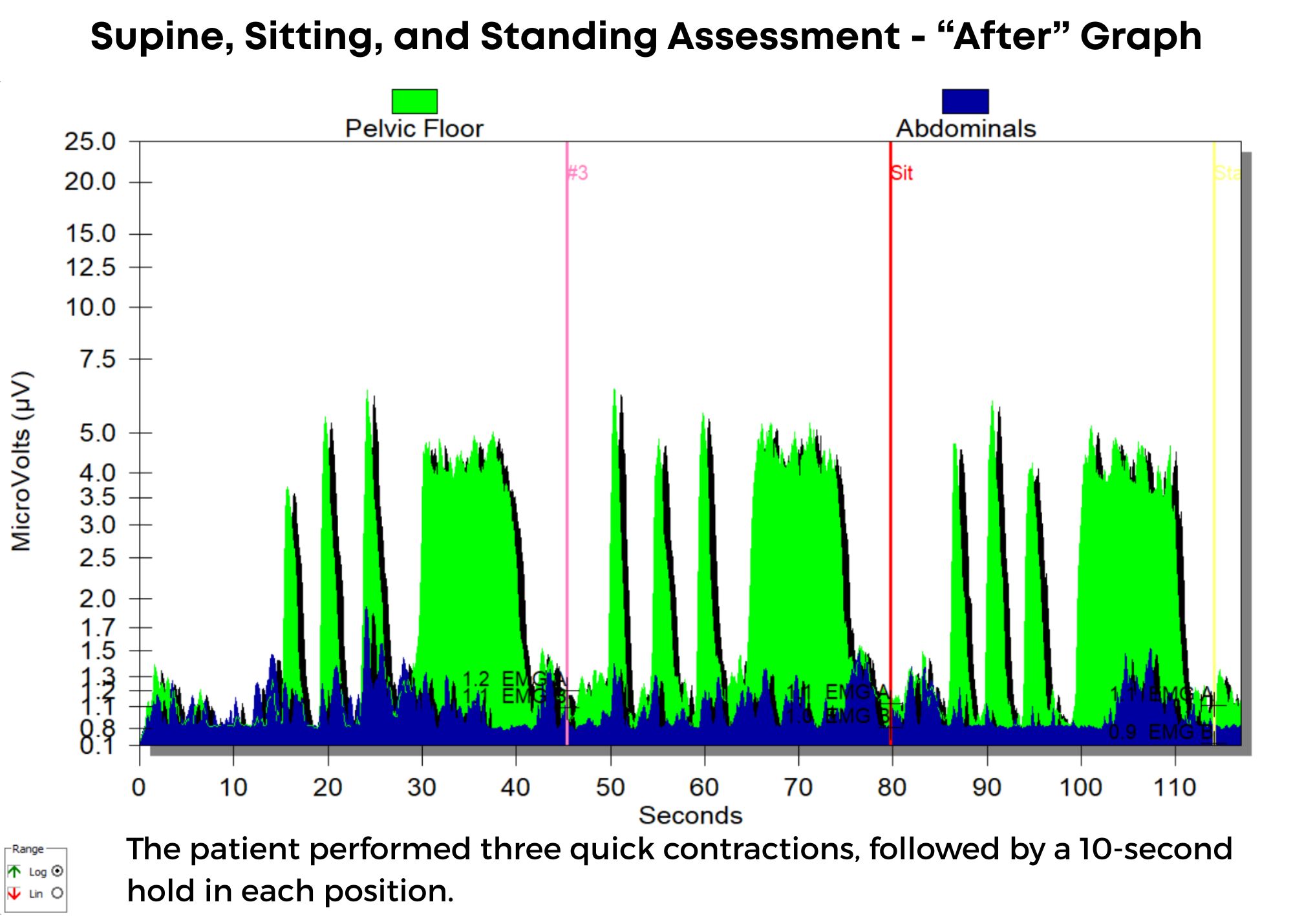
Conclusion
A long history of scientific evidence supports using sEMG biofeedback in managing incontinence or pain symptoms. As a noninvasive, cost-effective, and powerful treatment modality, healthcare providers should consider this tool when managing pelvic floor dysfunction. Providers should be educated in adequately using this valuable modality to gain the most out of the skills and knowledge achieved through this intervention. For more information regarding courses and certification, please visit www.pelvicfloorbiofeedback.com.
Biofeedback for Pelvic Muscle Dysfunction, a self-hosted lab course scheduled for May 4, 2025, is led by Instructors Kaufman and Lee who introduce participants to the use of biofeedback when treating bladder, bowel, and pelvic floor disorders. In this course, participants learn about surface EMG biofeedback by using the equipment on themselves to experience dynamic muscle assessment in supine, sitting, and standing positions. This dynamic course also includes behavioral strategies for relearning proper muscle control for improved pelvic floor function.
Instructors Kaufman and Lee have over fifty years of combined experience using this amazing clinical tool. This treatment approach uses sEMG biofeedback to visualize muscle dysfunction, then allows for proper training and education to re-establish proper muscle movement patterns, enabling patients to gain control over function and realize they can succeed in improving symptoms. Lee adds, “Patients are constantly validating the usefulness of this modality by reaping the benefits of skilled training and behavior modification strategies.”
References:
- Cram, J. R., & Kasman, G. S. (2011). The basics of surface electromyography. In E. Criswell (Ed.). Cram’s introduction to surface electromyography (2nd ed., pp. 3–7). Jones and Bartlett
- Kaufman, J., Stanton, K., & Lee, T. E. (2021). Pelvic Floor Biofeedback for the Treatment of Urinary Incontinence and Fecal Incontinence. Biofeedback, 49(3), 71-76.
- Shelly, Beth & Kaufman, Jane (2023). Foundations of Pelvic Floor Muscle Assessment Using Surface Electromyography. APTA Academy of Pelvic Health Physical Therapy.
- Szczygielska D, Knapik A, Pop T, Rottermund J, Saulicz E. (2022). The Effectiveness of Pelvic Floor Muscle Training in Men after Radical Prostatectomy Measured with the Insert Test. Int J Environ Res Public Health. 2022 Mar 2;19(5):2890. doi: 10.3390/ijerph19052890. PMID: 35270582; PMCID: PMC8910379.
AUTHOR BIO
Tiffany Lee, OTR, OTD, MA, BCB-PMD, PRPC
 Tiffany Lee holds a BS in OT from UTMB Galveston (1996), an MA in Health Services Management, and a post-professional OTD from Texas Tech University Health Sciences Center. In 2004, she received her board certification in Pelvic Muscle Dysfunction from the Biofeedback Certification International Alliance. She is a Herman and Wallace Pelvic Rehab Institute faculty member and teaches biofeedback courses. She has been treating pelvic health patients for 25 out of her 30-year career. Her private practice in San Marcos, Texas, is exclusively dedicated to treating urinary and fecal incontinence and pelvic floor disorders. Her continuing education company, Biofeedback Training & Incontinence Solutions, offers clinical consultation and training workshops. She also enjoys mentoring healthcare professionals working toward their BCIA certification.
Tiffany Lee holds a BS in OT from UTMB Galveston (1996), an MA in Health Services Management, and a post-professional OTD from Texas Tech University Health Sciences Center. In 2004, she received her board certification in Pelvic Muscle Dysfunction from the Biofeedback Certification International Alliance. She is a Herman and Wallace Pelvic Rehab Institute faculty member and teaches biofeedback courses. She has been treating pelvic health patients for 25 out of her 30-year career. Her private practice in San Marcos, Texas, is exclusively dedicated to treating urinary and fecal incontinence and pelvic floor disorders. Her continuing education company, Biofeedback Training & Incontinence Solutions, offers clinical consultation and training workshops. She also enjoys mentoring healthcare professionals working toward their BCIA certification.









































