If you have been following research in pelvic pain, you may be aware of the diagnostic terms interstitial cystitis (IC) as well as painful bladder syndrome (PBS). And there's always bladder pain syndrome (BPS), or hypersensitive bladder syndrome. While you may have heard at some point that health care providers should use PBS preferentially over IC, that recommendation does not seem to have stuck, and the Interstitial Cystitis Association (ICA) has decided to utilize "IC" until a more definitive diagnostic criteria and test are developed. Much of the literature you will continue to see published will choose to include both IC and PBS together in the title, and recent research has attempted to further define the diagnosis as having a relationship to ulcers versus no ulcers.
Recognized subtypes of IC include ulcerative (5-10% of those with IC) and non-ulcerative (90% of those with IC). According to the ICA, patients who have non-ulcerative IC have tiny glomerulations or hemorrhages on the bladder wall, indicative of inflammation, but not specific to IC. In patients who have ulcerative IC, Hunner's ulcer's or patches of red, bleeding areas are noted on cystoscopy. Recent research aimed to find out if female patients with ulcerative versus non-ulcerative IC have different symptoms or characteristics. 214 women (36 with ulcerative IC, 178 with non-ulcerative IC) were included in this research. While both groups reported triggers such as certain foods, exercise, and stress, more patients who had non-ulcerative IC reported pain with intercourse.
On the Brief Pain Inventory, one of the outcomes tools used in this study, both groups reported similar numbers of painful areas, with lower abdominal and pelvic pain followed by low back pain. Words used to describe the pain were, however, different among the two subtypes of IC: patients with non-ulcerative IC reported aching, cramping, and tenderness, while patients in the ulcerative group reported sharp, stabbing, and hot burning pain. Aside from these differences, the patients in the two groups did not share significant differences in the outcomes measured. The authors suggest that further research is needed to provide more information about the different presentations of patients who have IC/PBS.
For those of us in pelvic rehabilitation, the most important aspect of our care is to treat what is found, and that can only be accomplished through excellent examination and evaluation techniques. If you are interested in learning more about IC, the ICA website provides a wide array of tools for patients and providers. Until then, we will continue to see IC, PBS, BPS, and other abbreviations that point out that there is much yet to learn about this disabling condition.
Even if you currently are not treating male patients in your pelvic rehabilitation program, continue to read for critical information about testicular pathology. Any male patient (or family member, friend, or loved one) can present with a sudden onset of symptoms that require medical follow-up. Testicular pathology, as pointed out in this article from Medscape, can be benign or life-threatening. (If you are not able to view the article, you can first create a free user account for Medscape and then view the information. Medscape is also a great resource as they will send you weekly article reviews on various medical topics.) The article has images of testicular pathology throughout the presentation which can help in understanding the anatomy and pathology present. Following are a few diagnoses that are highlighted in the article, and that may mimic clinical symptoms of thoracolumbar radiculopathy or pelvic pain.
Testicular torsion: Commonly occurring in adolescent males, torsion happens when the testicle twists, impairing the blood flow to and from the testicle. If the twisting last 4-6 hours or longer, the testicle can become necrotic and no longer be viable. Pain, swelling, and erythema are common in this condition, and any patient who presents with acute onset of scrotal pain must be examined for this condition.
Testicular fracture: Blunt trauma can cause significant injury to the testicles, and conservative management may be all that is required. The testicle itself can fracture, or be degloved, and a significant hematoma can occur. Surgical intervention may be required for preservation of the testicle.
Hydrocele: Fluid can collect either in the scrotum or in the spermatic cord (the "tube" that extends from the lower abdominal wall to the scrotum, carrying neurovascular and other structures). A painless lump may be the first sign of this condition. Aspiration or surgical resection may be required.
Varicocele: An enlargement of the veins within the scrotum can lead to a varicocele. While this may not cause dysfunction for the patient, a varicocele can lead to infertility and possibly discomfort due to the dragging sensation and increased pressure from enlargement.
Epididymitis: Testicular swelling, redness, and tenderness may be caused by an infection to the epididymis, a structure within the scrotum. A patient who presents with these symptoms may also have a fever and should be evaluated medically.
In addition to the above diagnoses, a testicular tumor might be first noted as a firm, painless nodule in either testicle. According to the Medscape article, a testicular tumor is the most common solid tumor found in men ages 20-35. Men need reminders just as women do for completing testicular self-exams and reporting any concerns to the physician. Here is a link to information on testicular self-exams, in case you find it helpful for patient education purposes. Keep the above information in mind when a patient presents with a change in symptoms or sudden, severe pain in the testicles.

The first ever Herman & Wallace course in the United Arab Emirates wraps up next week, and the Institute is eagerly looking forward to brining our mission to some other exciting international locations in the next few months.
In early January, Herman & Wallace faculty member Michelle Lyons will be teaching Oncology and the Pelvic Floor, a course covering gynocological, colorectal, prostate and testicular cancers and current cancer treatments and their implications for the pelvic floor at Mullingar General Hospital in Westmeath, Ireland.
Following that course, Michelle will be traveling to Kuwait City, Kuwait to teach a similar seminar to a group of women's health physiotherapists. The Kuwait course will focus on Oncology and Women's Health and will cover gynocologic, colorectal and breast cancer treatment.
In February, Michelle will return to Ireland to teach Herman & Wallace's Pelvic Floor Level One course at the School of Health Sciences at the University of Ulster.
We are so proud to have an international faculty member spreading the pelvic rehab gospel across the globe!
If you would like to catch Michelle teaching stateside, she will be instructing Care of the Pregnant Patient in Houston, TX in April and Care of the Postpartum Patient in Salt Lake City in October, two courses she helped develop with the rest of our team of faculty Pregnancy and Postpartum experts, or, as we call them, "Preg-perts". These courses are brand new in 2013 and we are excited to be offering these expanded course topics!

The Women's Action Initiative is an organization whose mission is to "empower women to prioritize pelvic and perinatal health as an integral element of their overall well being and quality of life". Founded in 2008 by Angela Hughes Halliwell, a mother of two, the WAI is currently waging a campaign to combat the effects of obstetric fistula in the Democratic Republic of Congo.
Currently, millions of women in the Congo are living with unrepaired obstetric fistula caused by inadequate medical care during labor and delivery. The consequent tearing between the vagina and bladder, the vagina and rectum, or both causes leakage between the tissue that results in urinary and fecal incontinence.
Women with fistula are often mocked, ridiculed and isolated for their incontinence, and are sometimes abandoned by their families and husbands.
The WAI is currently raising money to send a team of three women's health physical therapists and a urogyn surgeon to Goma to treat, rehabilitate and educate these women. Their goal is to raise $50,000 for this endeavor.
Herman & Wallace support this mission and has made a donation towards this project. If you would also like to donate, you can do so here.

Institute founder and faculty member Holly Herman is jet-setting yet again! This time, she is teaching an 11-day intensive seminar on women's health and pregnancy and postpartum for physiotherapists in Dubai, United Arab Emirates.
There are 26 participants in this course, all of them women, who hail from India, Pakistan, Baharain, Indonesia, UAE, Saudi, UK, and Oman.
The intensive course will cover topics from Herman & Wallace's Pelvic Floor Level 1, 2A and 2B and 3 courses, as well as our Pregnancy and Postpartum series of courses. For the first time ever this country, female physiotherapists will learn internal evaluation and treatmetn techniques for female patients, as well as using biofeedback to assess pelvic floor patients.
We are elated to be able to bring the mission of the Institute to such a broad audience across the globe!

With the Thanksgiving holiday behind us, the concept of gratitude may be fresh in our minds. Choosing to live with gratitude is often correlated with positive health benefits, such as increased energy, optimism, and empathy, according to the Psychology Today website. Most of us in the healing professions find reward in our work because of the expressed appreciation of others, and we can all tell meaningful stories about the patients who touched our own hearts with their thanks. Such support can boost our own energy levels and help us get through the paperwork or the more difficult patient encounters.
Gratitude, or thankfulness, invites a person to reflect on the aspects of her life that are providing meaningfulness. It is not necessary to be thankful only for the gifts that life brings; a person may also be grateful for a challenging interpersonal experience or life event as we often learn significant lessons during those times. There are abundant resources to encourage the building of a gratitude-filled life, and most of them are quite simple, require very little in terms of investment, and are described as methods that can change a person's outlook and improve quality of life.
According to an article written by Randy and Lori Sansone (click here for full text of the article), both psychologists, an attitude of gratitude can be cultivated by:
- Keeping a journal with entries listing statements of things you were grateful for during the day or week
- Thinking about a person for whom you are grateful (I would add "or a pet" as so many people have wonderful animal companions)
- Writing or sending a letter to someone who you are grateful towards
- Meditating on gratitude
- Completing a "Count Your Blessings" exercise
- Practicing saying "thank you" with sincerity and meaning
- Writing thank you notes
- Being prayerful about gratitude
While our patients may enjoy and benefit from discussions about the above, especially when working towards healing from chronic pain issues, there are many benefits to be gained in many domains of life. For example, gratitude has been described as being important for maintaining intimate relationships, encouraging prosocial behavior by helping others to feel socially valued, and improving job satisfaction. Click here for an excellent article about gratitude and being appreciated in the workplace (and what to do if you do not feel appreciated.)
There is even an app called HappyTapper that allows you (or a patient) to write down five things each day for which you are grateful. If that's not enough to be thankful for, it only costs 99 cents! There are also several free online journals available if you search the terms "free gratitude journal." With the holiday season and the New Year approaching, talk tends to turn to items desired and wishes for a healthier, better body and changes in income or relationshp. What would it sound like if we chose instead to focus on all that we already have and express our gratitude? In the words of physician Christiane Northrup, "Feeling grateful or appreciative of someone or something in your life actually attracts more of the things that you appreciate and value into your life." As we enter the holiday season, and winter, a time of turning inward, may you attract more wonderful things into your life.
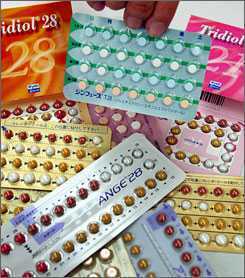
In a new committee opinion, the American College of Obstetricians and Gynecologists (ACOG) wrote that birth control pills should be sold as an over-the-counter drug, meaning "the pill" would be available to women without a doctor's prescription or a preliminary medical examination.
According to ACOG, unintended pregnancies accounted for 50% of all American pregnancies in the past 20 years, a rate that is "unacceptably high", according to ACOG. According to the Institute of Medicine, women with unintended pregnancy are "more likely to smoke or drink alcohol during pregnancy, have depression, experience domestic violence, and are less likely to obtain prenatal care or breastfeed. Short interpregnancy intervals have been associated with adverse neonatal outcomes, including low birth weight and prematurity, which increase the chances of children’s health and developmental problems."
"A potential way to improve contraceptive access and use, and possibly decrease the unintended pregnancy rate, is to allow over-the-counter access to [oral contraceptives]," the Committee on Gynecologic Practice wrote in the opinion.
Concerns regarding the use of birth control pills include their being linked to increased risk of blood clots and venous thromboembolism (VTE), a potentially deadly condition. The committee says that the risk is, however, "extremely low" and that only 3 out of every 10,000 women using oral contraceptives experience VTE, lower than the rate of women who experience VTE while pregnant or after having just given birth. (Abstract). ACOG says that women should self-screen for most contraindications to oral contraceptives using checklists and that a doctor's screening should not be required.
Other concerns cited are that, when no longer required to visit a doctor in order to obtain a prescription, many women will not receive the pelvic exams, pap smears and STD tests which they would typically receive when seeing a doctor to obtain birth control.
While ACOG asserts that making birth control available over the counter will lower the over-all cost of the pills (on average, uninsured American women spend $16 a pack for the pill) some worry that, when no longer covered by insurance as a prescription drug, the cost of their birth control will actually go up.
This opinion, though ground breaking, is unlikely to change the way oral contraceptives are dispersed in the immediate future. Changing the availability of birth control pills would require drug companies to seek permission from the government to sell the pills without a prescription, and it is unclear if any companies will do so.
With PF1 Durham just around the corner, and PF1 Seattle in January sold-out with a 20-person wait list, our next PF1 is filling up quickly.
PF1 in Maywood, IL from March 1-3 is over half-full, and additional registrations are rolling in each day. If you are interested in joining us for PF1 in Maywood, do not hesitate to register. We expect this course to fill up before the holidays are upon us, so act quickly.
Once PF1 in Maywood is full, the next available PF1 is in Houston, TX in early May 2013. If you'd like to take this popular course before May of 2013, we suggest registering for the Maywood course today!
Stay tuned this week for a big announcement that we have coming up. We are adding a new highly requested feature to our website, which we are confident women's health physical therapists will find very helpful!

Congratulations to Herman & Wallace faculty member, Peter Phillip, who was recognized in his community for his stellar work as a therapist. The New Canaan Advertiser writes, "if you end up at Philip Physical Therapy on Vitti Street, you’re in good hands". (Read the full article HERE)
Peter developed two courses which he instructors through Herman & Wallace, Sacroiliac Joint and Pelvic Ring Evaluation and Treatment and Differential Diagnostics of Chronic Pelvic Pain: Interconnections of the Spine, Neurology and the Hips. Peter is also an item writer and Subject Matter Expert developing our Pelvic Therapy Practitioner Certification Exam.
Way to go, Peter!
"Movember," a men's health movement that began in Australia, has found its way around the globe. In this campaign, men grow mustaches (starting out November 1st clean-shaven) for one month to raise awareness about men's health issues, with particular emphasis on prostate and testicular cancer. Check out some of these images on the website to see for yourself how awesome these staches are.
This is a serious fundraising effort- in 2011 the organization raised over 126 million in US dollars. This money is spent on increasing awareness of male cancers and also on improving the response of the medical community to these conditions. Funds are also directed to organizations such as The Prostate Cancer Foundation.The organization's strategic goals as outlined on their website are to fund survivorship initiatives, increase awareness and education, fund research including clinical trials and research that informs health policy. The first item on the group's list of values is "fun" and we can easily see why this event attracts repeat crowds.
So what if you can't grow a mustache? You can still attend a Movember event sporting a faux such as a mustache-on-a-stick. Learn how to make your own here. Women engaged in the movement are known as Mo Sistas, and certainly men's health issues are issues for all families, as are women's health issues. In the presence of cancer, as we know, early detection can improve survival and allow for more treatment options. If you would like to find an event near you, check out this interactive map. If you live in Seattle or in Orange County, you can attend a "Running of the Mo's" event!
Regardless of your level of participation, what a terrific organization to celebrate and share with others. Consider hosting or attending a Movember event, and consider engaging someone in a dialog about men's health screening as well as pelvic rehab options. (Mustache optional.)
By accepting you will be accessing a service provided by a third-party external to https://hermanwallace.com./










































