
We are pleased to announce the following changes and additions to our core series of courses. These changes are being undertaken by our Curriculum Development Team based on evolving realities of our field and the body of evidence and literature. In keeping with the way the field has evolved, we will be making the following changes to our core coursework.
Two courses will be joining our Pelvic Function Series:
- Pelvic Function Modalities - This brand new course is an in-person two-day continuing education course targeted to pelvic health clinicians covering frequently used modalities in pelvic health, including biofeedback and EStim. Hands-on labs using a variety of equipment necessitate that this course be offered in-person, where participants can practice using the equipment.
- Pelvic Function Level 2C: the Male Pelvic Floor and Men’s Pelvic Health - formerly the stand-alone course, Male Pelvic Floor Function Dysfunction and Treatment, this course is now being adapted and reformatted to be a part of the Pelvic Floor Series, reflecting the inclusive stance of H&W core series instructing in the care of all patients. This course will be offered as satellite, self-hosted, and in-person options in order to provide the most flexible pathway for participants.
In addition to these two new offerings, you will see greater inclusion of all genders throughout the series, starting with PF1. The modified titles and topics will be as follows:
Pelvic Function Level 1: Introduction to Pelvic Health - this course will provide a thorough and comprehensive introduction to anatomy and physiology of the pelvis and surrounding structures in all genders. Includes an introduction to performing intra-vaginal exam. This course will be offered in satellite and in-person formats.
Pelvic Function Level 2A: Colorectal Pelvic Health and Pudendal Neuralgia, Coccyx Pain. In labs, anorectal internal exam will be introduced. This course will be offered in satellite and in-person formats.
Pelvic Function Level 2B - Urogynecologic Topics in Pelvic Health. This course will be offered in satellite, self-hosted and in-person formats
Pelvic Function Series Capstone - Integration of Advanced Concepts in Pelvic Health. This course will remain targeted to the advanced clinician. A greater emphasis on workshopping clinical case studies will be incorporated. This course will be offered in satellite, self-hosted and in-person formats.
Questions:
What courses will be required in order to advance to the Capstone course?
As we understand the “advanced pelvic floor clinician” may have a variance of experience and focuses, the following course “journeys” can all be taken in order to take the Capstone course:
PF1
PF2A
P2B and/or PF2C
The Modalities course is strongly recommended, but not required, in order to take the Capstone course.
Why is the series being expanded and updated in this way? .
It is a reality of our field that pelvic rehab evolved from a tradition of “women’s health physical therapy”, and that is reflected in the vulvovaginal emphasis of the current coursework. As the scope of pelvic rehab has expanded to encompass men’s health and care for all genders, it is important that all pelvises be incorporated at every level of our series, and that men’s health be a foundational part of our curricula, rather than being siloed as a specialty offering.
I have already started my PF series coursework, where do I go now?
If you have taken only PF1, you should advance to PF2A, 2B or 2C in any order. You may also wish to take the Modalities course in order to learn evidence-based use of modalities and practice biofeedback and Estim in a hands-on, in-person setting. The best way to choose which course to take next will be determined by who shows up in your clinic after completing PF1 and beginning to see your first pelvic patient caseload.
If you have taken PF1 and 2A - take either 2B or 2C or both in any order to advance to Capstone. If you took PF1 following the pivot to the satellite model, you may also wish to take the Modalities course in order to practice hands-on biofeedback and Estim labs.
If you have taken PF1 and 2B, you must take 2A prior to Capstone. You may take the 2C course to learn men’s health topics if seeing male and male-identifying patients is part of your clinical goals. If you took PF1 following the pivot to the satellite model, you may also wish to take the Modalities course in order to practice hands-on biofeedback and Estim labs
If I have taken PF1, 2A, and 2B - you may advance to Capstone or you may take the 2C course to learn men’s health topics if seeing male and male-identifying patients is part of your clinical goals. If you took PF1 following the pivot to the satellite model, you may also wish to take the Modalities course in order to practice hands-on biofeedback and Estim labs
If you have taken PF1, 2A, 2B and Capstone but have not taken the former Male Pelvic Floor course, you may take the 2C course to learn men’s health topics if seeing male and male-identifying patients is part of your clinical goals.
If you have taken PF1, 2A and the Male Pelvic Floor course, you may advance to Capstone
If you have taken PF1, 2A, 2B and the Male Pelvic Floor course, you may advance to Capstone
Am I required to take more courses in order to complete the PF series now?
No. Previously, there were three prerequisite courses for taking the advanced Capstone course: PF1, 2A and 2B. Following the changes to the series, the prerequisite courses for taking Capstone will be PF1, 2A and 2B OR 2C (or both, depending on one’s target patient population). The Modalities course is a strongly encouraged, but not required, level of the PF series.
As before, participants should choose their next course based on the patient needs they are seeing in the clinic. Following PF1, many may see patients with fecal incontinence or coccyx pain and may choose to prioritize PF2A as the next step in their journey. Others may see patients with penile pain or incontinence post-prostatectomy and may choose to take 2C as their next step.
As before, there are no required courses in order to sit for the Pelvic Rehab Practitioner Certification Exam.
Why aren’t there self-hosted options for PF1 and PF2A?
PF1 is most learners’ first introduction to performing intra-vaginal assessment and therefore we believe the best learning experience will be under the guidance of either an HW faculty member or trained teaching assistant at an in-person or satellite course. Similarly, PF2A is most learners’ first experience performing anorectal exam, which should also take place under the supervision of an experienced clinician. In PF2B, 2C, and Capstone, these techniques are refined and it is therefore appropriate to allow self-hosted options for those who have already learned these skills and are comfortable with independent learning.
I see that there will be options for a few in-person as well as satellite offerings for much of the series. Will HW continue to offer both formats?
We understand that many people appreciate the flexibility and accessibility of the satellite model as an improvement over the days when all series courses were sold out with long waitlists and lengthy travel was often required to attend our courses. We also understand that some folks simply prefer the format in which instructors are present at the course. Our intention is to offer formats that accommodate everyone’s needs, which is why the PF series will be available in-person as well as in the satellite format starting in 2024. Because of the hands-on equipment needs of the Modalities course, this will be available exclusively in person.
Why is PF1 required for 2C if it wasn't for MPF?
Historically, the Male Pelvic Floor course was a stand-alone course, meaning that many participants would take this course after beginning their journey with PF1 and after already seeing patients with pelvic floor dysfunction. Others, often male and male-identifying practitioners who did not feel their goals were met by the vulvovaginal-centered PF series, would take the Male course as their first ever introduction to pelvic health. This resulted in course attendees being in vastly different places in terms of experience, which often results in a sub-optimal learning experience for all.
As part of our push to see more information about patients of all genders incorporated at every level of the core series, PF1 which contains foundational information on all pelvises and core concepts in pelvic rehab, will be a prerequisite for 2C, which will build on those core concepts as they apply specifically to the male and male-identifying patient.
Who can act as a Teaching Assistant for the series courses in the new format?
PF1 - must have PF1, and ⅔ of the Level 2s (2A, 2B, and 2C)
PF2A - must have 1, 2A, and 2B or C
PF2B - must have 1, 2B
PF2C - must have 1 and have taken the Male Pelvic Floor in 2016 or later
Capstone - must have 1, 2A, 2B or 2C, and Capstone

Herman & Wallace is committed to providing courses on pelvic rehabilitation for all people across the spectrum. This week the featured courses are those focused on women's health!
Take a look and see if there is one that is a good fit for you.
Breastfeeding Conditions Remote Course - Remote Course
July 16 and November 19

This course provides a thorough introduction to the physiology of the lactating breast, dysfunction and treatment interventions, the therapist's role in breastfeeding and pumping support, as well as when to refer to other health professionals.
Lectures will include the anatomy and physiology of lactation, blocked ducts and mastitis, and breast pain through a biopsychosocial lens. During labs, participants will have the opportunity to systematically assess the breast and practice therapeutic breast massage and manual milk expression. Participants will learn to assess and treat breast inflammation and pain such as mastitis, blocked ducts, milk blebs, and cracked nipples.
Breastfeeding Conditions - July 16-17, 2022
Breastfeeding Conditions - November 19-20, 2022
Menstruation and Pelvic Health - Remote Course
July 16-17, 2022

Menstruation and Pelvic Health is a two-day remote course is designed for clinicians who want to obtain advanced knowledge and skills to educate patients on non-hormonal, non-surgical, and non-prescription interventions for improving the Menstrual Experience. Developed by Nicholas Gaffga, MD, MPH, FAAFP, and presented together with Amy Meehan, PT, DPT, MTC, this course is geared toward the pelvic rehab provider looking to impart Menstrual Interventions that:
- Put control in the hands of people who menstruate to identify and carry out the interventions that are appropriate to them
- Use a holistic approach and advanced knowledge and familiarity with body and mind
- Emphasize healthy practices that can positively impact the Menstrual Experience and beyond, in areas such as mental health and chronic diseases
- Discover root causes of issues, rather than quick fixes, to have benefits that are sustainable across the lifespan.
Postpartum Rehabilitation - Remote Course
offered monthly through November

The client who is postpartum may be one of the most overlooked clients in health care. Knowing the specific rehabilitation needs to help with common problems and prevent future problems is the goal of this beginner-level course. For the orthopedic-based practitioner, this course will solidify awareness of the common orthopedic needs of the postpartum client. For the non-orthopedic practitioner, this course will provide a foundation for working with clients experiencing common postpartum-related musculoskeletal conditions.
This course will cover examination considerations and modifications specific to postpartum, as well as specific questions to ask during history taking and methods for identifying red flags in postpartum. More comfortable positions during the examination/treatment and common posture/gait/balance changes during postpartum are covered. The participant in this course will understand necessary biomechanics training for daily activities, child care, and breastfeeding. As an expansion from the pregnancy rehabilitation course, participants will be taken through progression in diastasis rectus abdominis (DRA) assessment and rehabilitation, including DRA exercises in lecture and lab.
Postpartum Rehabilitation - July 23-24, 2022
Postpartum Rehabilitation - August 20-21, 2022
Doula Services and Pelvic Rehab Therapy - Remote Course
August 6 and December 10

A growing number of pelvic health therapists are recognizing the importance of preparing their clients for the physical and mental challenges of labor and delivery. In some cases, this is extending to a desire to be present during labor for support as a Doula. The purpose of this course is to present the unique challenges of merging a rehab practice with Doula services in order to help the participant better discern whether or not this is a journey worth taking.
Doula Services and Pelvic Rehab Therapy - August 6, 2022
Doula Services and Pelvic Rehab Therapy - December 10, 2022
Fertility Considerations for the Pelvic Therapist - Remote Course
August 13

This course is for practicing pelvic rehabilitation therapists and covers the role of rehabilitation therapists in optimizing female fertility. This course was written and will be instructed by Dr. Yeni Abraham, who is a Dallas-Ft.Worth-based Pelvic Physical Therapists specializing in the treatment of Gynecologic and Fertility related conditions. Lecture topics include medical infertility labs, pertinent information on charting cycles, assisted reproductive technologies and their impact on treatment, hormone regulation, the relationship between inflammation and infertility, amongst other topics. Lab activities/break-out sessions will include manual techniques to influence uterine and ovarian Mal-positions.
*This course will require that each student have a live model that will allow participants to practice the lab techniques on a human body. Due to the nature of labs, please be sure your model partner is not pregnant and does not have an IUD for safety. Additionally, those with hydrosalpinx will not be able to participate in uterine mobility techniques but can still attend the course.
Fertility Considerations for the Pelvic Therapist - August 13, 2022
Menopause Transitions and Pelvic Rehab - Remote Course
August 27-28th and November 12-13th

Menopause Transitions and Pelvic Rehab is a two-day course is designed for the clinician that wants to understand the multitude of changes that are experienced in the menopause transition and how they affect the aging process. Upon completion of this course, participants will have a basic understanding of the hormonal changes during menopause, the impact on various health systems, and interventions that can assist with improving this transition.
This is an excellent opportunity to understand the physiological consequences to the body as hormones decline, in order to assist our patients in lifestyle habits for successful aging. Topics will include cardiovascular changes, metabolic syndrome, bone loss and sarcopenia, neurological changes (headache, brain fog, sleeplessness), Alzheimer’s risk, and urogenital changes. Symptoms and treatment options will also be discussed, including hormone replacement, non-hormonal options, dietary choices, and exercise considerations.
Menopause Transitions and Pelvic Rehab - August 27-28, 2022
Menopause Transitions and Pelvic Rehab - November 12-13, 2022
Medical Perspective in Peripartum Care - Remote Course
September 17-18th
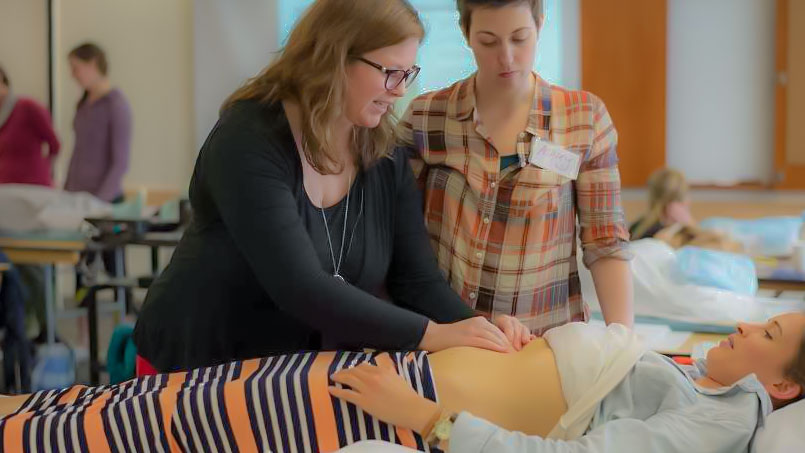
Medical Perspective in Peripartum Care is a two-day course instructed by Dina Gordon, MD, FACOG, a practicing OB/GYN in the Seattle area, and will discuss common conditions encountered in the peripartum period from the medical perspective. Topics include medical screening; medical management of high-risk patients (bed rest, activity limitations, medications, surveillance); and interventions common in the peripartum period
The course is built from the medical perspective, the design of the course aims to share knowledge so that rehabilitation care planning is optimized.
Medical Perspective in Peripartum Care - September 17-18 2022
Pregnancy and Postpartum Considerations for High Intensity Athletics
September 11

The main focus of this course will be to learn how exercising throughout pregnancy, or returning to exercise postpartum may look different for a high-intensity athlete versus a non-HIIT athlete. Participants will discuss how anatomical and hormonal changes affect training for the pregnant and postpartum athlete, review various modifications for this population, learn how various stresses placed on the body during these activities may affect pelvic floor muscle function, and review various pressure management strategies that can be utilized during high-intensity interval training. This one-day remote continuing education course is designed to educate practitioners on the unique considerations of pregnant and postpartum athletes engaging in high-intensity interval training (HIIT).
During the pregnancy lab, we will review specific exercise modifications for pregnancy, utilization of breathwork to properly support the pelvic floor during pregnancy and review how to assess for and tape for diastasis recti. In the postpartum lab, we will review how to determine proper activity modification based on the ability to manage pressure, review specific activity modifications and breathwork, review accessory work for return to activity, and discuss how to assess pelvic organ prolapse in standing.
Pregnancy and Postpartum Considerations for High Intensity Athletics - September 11, 2022
Perinatal Mental Health: The Role of the Pelvic Rehab Therapist
October 22

This one-day continuing education course covers mental health considerations during pregnancy and postpartum and is targeted to the pelvic rehab clinician treating patients in the peripartum period. Topics include common mental health concerns in the postpartum period including depression, anxiety, OCD, and PTSD, as well as the connectedness between mental health and physical dysfunction.
The course will introduce useful screening tools and how to connect patients to resources and diagnosing professionals. Labs will include partnered breakout sessions to practice listening and dialogue skills. The course also includes a review of coping techniques to support mental health and physical symptoms.
Perinatal Mental Health: The Role of the Pelvic Rehab Therapist - October 22, 2022
Pregnancy Rehabilitation - Remote Course
October 29-30 and November 5-6

Learn how to safely examine and treat the pregnant patient in this beginner-to-intermediate course.
Lectures cover terminology, fertilization, trimesters, medical testing/interventions, imaging, and medications. Participants will learn to differentiate between false labor, progressive labor, and other musculoskeletal pain as well as learn to understand typical hormonal and systemic changes during pregnancy. Examination, evaluation, and treatment of common lumbopelvic conditions will be provided with an introduction to diastasis rectus abdominis, pelvic floor dysfunction, breathing, and deep core assessment/treatment.
Discussions also include general examination considerations and modifications specific to pregnancy, including a discussion of modalities and manual therapy techniques considered safe or precautioned during pregnancy, with further lectures on pelvic girdle examination, diagnosis, and treatment strategies. Finally, to prepare the pregnant client for labor and birth, instruction in perineal stretching, hip and trunk flexibility activities and TENS for labor will be discussed. Lab practice will include labor and birthing positions, with a focus on consideration for positional strategies for women with pre-existing musculoskeletal problems.
Pregnancy Rehabilitation - October 29-30, 2022
Pregnancy Rehabilitation - November 5-6, 2022
Faculty member, Ginger Garner PT, L/ATC, PYT will be giving 2 lectures at this year’s annual Montreal International Symposium for Therapeutic Yoga, or MISTY for short, in Montreal, Quebec. The first is a 2-hour lecture titled, Vocal Liberation, and the second is a 4-hour lecture titled, Hip Preservation: Yoga Reconsidered, Visit http://www.homyogaevents.com to learn more.
 Yoga is, unarguably, a popular contemplative science, enjoying 36.7 million practitioners in the US alone, up from 20.4 million in 2012.1 A 16 billion dollar industry, yoga is one of the most widely utilized methods of complementary and integrative medicine in America today. In 2008, the editor of Yoga Journal declared “yoga as medicine” as the next great wave. That was right in the middle of the Great Recession, when the last thing on the collective healthcare industry’s mind was yoga.
Yoga is, unarguably, a popular contemplative science, enjoying 36.7 million practitioners in the US alone, up from 20.4 million in 2012.1 A 16 billion dollar industry, yoga is one of the most widely utilized methods of complementary and integrative medicine in America today. In 2008, the editor of Yoga Journal declared “yoga as medicine” as the next great wave. That was right in the middle of the Great Recession, when the last thing on the collective healthcare industry’s mind was yoga.
What happened during the same time frame as the interest in yoga surged?
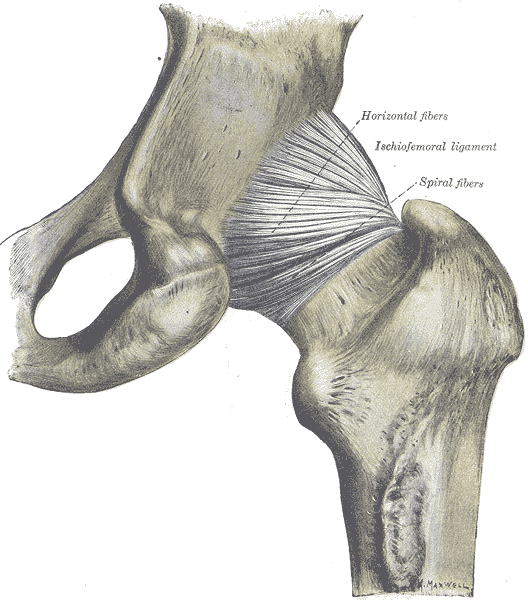
Our expanded knowledge of hip anatomy, physiology, and pathophysiology exploded onto the medical scene, providing more information than ever about how to address, preserve, and otherwise attend to the hip joint. Prior to this new age of research, the hip was relegated to a joint worthy of no more than a tendonitis, bursitis, or osteoarthritis diagnosis. A person was simply a hip replacement candidate or not. There was no other option once a hip joint had prematurely degenerated. Now, that has all changed, thanks to technological advances in diagnostic testing and investigation.
Yet, the worlds of hip preservation and rehabilitation and yoga have yet to join hands. Many of my patients and colleagues have suffered from unnecessary hip injuries, from labral tears, all types of impingement, and compounding secondary diagnoses such as torn hamstrings, sports hernias, gluteal tendinopathy, to pelvic pain, all due to yoga practice. Some suffered injuries in yoga class during a single traumatic injury, and some injuries were drawn out over years of accumulated microinjury to capsuloligamentous, bony, or cartilaginous structures.
Hip labral injuries (HLI) have vastly increased over the last 10 years, perhaps making HLI the newest orthopaedic diagnosis of the 21st century. This discovery also makes surgical and conservative management of HLI uncharted territory. Conservative therapy includes nonsurgical and post-surgical rehabilitation, and since the average time from injury to diagnosis is 2.5 years, there are many people with hip, pelvic, back, or sacroiliac joint pain that have undiagnosed hip labral tears.
I should make myself quite clear, however. I am not out to demonize yoga or fear-monger the practice of yoga or how it may wreck a person’s body (to use recently controversial language).
My purpose is two-fold: To clarify 1) “what” and “how” yoga can be a safe, effective form or physical therapy and rehabilitation for the hip and pelvis, as well as to 2) underscore the areas where yoga posture practice should be evolved to prevent injury.
To that end, I have written and will be presenting a new 4-hour workshop entitled, Hip Preservation: Yoga Reconsidered, at the Montreal International Symposium on Therapeutic Yoga (MISTY) this weekend in Canada. The lecture is relevant for yoga teachers, yoga enthusiasts, yoga therapists, and health care professionals who are interested in learning how to prevent hip injury in yoga practice.
The workshop will introduce identification of imbalances that could contribute to HLI, as well as understand the common mistakes made in yoga practice that could increase HLI or hip impingement. Understanding the pain patterns that surround HLI are also critical to safe and therapeutic yoga practice and will be discussed. Discussion of structure, function, ability and “dis”ability of the hip, including their major substrates, will help identify the “red flags” in yoga practice, identifying high risk populations and those who need postural modification(s) and/or outside referral to physical therapy.
I am looking forward to instructing a high energy, action-packed hands-on learning session at MISTY on March 19-20, along with my presenting a 2-hour lecture on maximizing public speaking impact through Vocal Liberation: The Voice as Therapy.
- The Voice as a Linking Science for Clinical and Business Efficacy
- Hip Preservation: Yoga Reconsidered
- Ginger’s lecture overview - Montreal International Symposium for Therapeutic Yoga
Want to learn more?
Bring Ginger’s 16 hour continuing education course, Differential Diagnosis for Hip Labral Injuries to your facility in 2017 through Herman & Wallace Pelvic Rehabilitation Institute.
Yoga in America 2016 Survey. Yoga Alliance and Yoga Journal. January 2016.
There's a lot going on in the world of pelvic rehab, and continuing education is no exception! This March, Herman & Wallace is hosting NINE courses around the country. It's a lot to keep up with, so we thought you might appreciate a brief overview of what's coming up next!
Where's this pain coming from?
Pelvic pain can have many sources, and Elizabeth Hampton wants to help you quickly get to the source. Finding the Driver in Pelvic Pain empowers you to play detective in order to help even the most complex patients. Don't miss out on Finding the Driver in Pelvic Pain in San Diego, CA on March 4-6, 2016
What goes in eventually comes out
How important is a good diet? For most of us eating healthy is important, and for many pelvic rehab patients it is a necessity. That's why Megan Pribyl wrote her "Nutrition Perspectives for the Pelvic Rehab Therapist" course. This beginner level course is intended to expand the your knowledge of the metabolic underpinnings for local to systemically complex disorders. Don't miss out on Nutrition Perspectives for the Pelvic Rehab Therapist - Kansas City, MO - March 5-6, 2016!
There's fascia everywhere!
Fascial mobilization is a rising star in pelvic rehab treatment techniques, and Ramona Horton is excited to share it with you! "Mobilization of the Myofascial Layer: Pelvis and Lower Extremity" is the best opportunity you'll get to learn about the evaluation and treatment of myofascia for pelvic dysfunction. Check it out on our continuing education course page. Ramona will be teaching these techniques in Santa Barbara, CA on March 11-13.
Giving birth hurts
Sometimes the newborn is the one to get all the attention, but what about the new mother? Be sure that you can help postpartum women with symptoms like postural dysfunction, pelvic girdle dysfunction, diastasis recti abdominis and more by attending Care of the Postpartum Patient in Seattle, WA this March 12-13, taught by the wonderful Holly Tanner!
Vulvar pain is easy to have and hard to lose
12% of women in the US have vulvar pain for 3 or more months at some stage in their life. It takes a multidisciplinary approach to address all the causes and co-morbidities, and that is exactly what you'll get at Dee Hartmann's Vulvodynia: Assessment and Treatment in Houston, TX on March 12-13, 2016. Dee aims to address the vicious cycle of pain, visceral and sexual dysfunction, and the general hit to quality of life that patients with vulvodynia suffer from.
The challenge of SI joint pain
The sacroiliac joint, pelvic girdle, and pelvic ring sure can take a beating, and Peter Philip knows how to keep you moving. Through exercise and stabilization, the pelvic rehab practitioner can quickly treat pain in the lumbopelvic-hip complex. Learn all about the direct and indirect anatomy that influences the sacroiliac joint, and then get ready to find and treat the source of pain and dysfunction in Sacroiliac Joint Treatment in Minneapolis, MN on March 19-20, 2016.
Taxes and Menopause
The menopause transition is not something many people look forward to. For some women it goes more smoothly than others, and it's the less fortunate ones who need access to a well-trained pelvic care professional. Michelle Lyons is flying in from Ireland to help you to become that pro! Be it vaginal atrophy, sexual health dysfunction, pelvic organ prolapse, or any other of the myriad possible symptoms of menopause, you'll be equipped to handle them all after attending Menopause: A Rehabilitation Approach in Atlanta, GA on March 19-20, 2016.









































