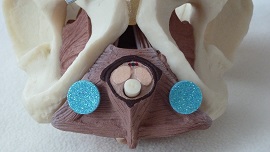
The American Heart Association/American Stroke Association Guidelines for Prevention of Stroke in Women reports that although stroke is not common during pregnancy, pregnant women are more at risk for stroke than non-pregnant young women. The guidelines describe the pregnancy-related physiologic factors of venous stasis, lower extremity edema, and blood hypercoagulability as factors in increased risk of stroke. Hypertensive disorders during pregnancy including preeclampsia can also increase maternal and fetal risk, with risk factors of obesity, age over 40, multiple pregnancy, and diabetes.
Postpartum hypertensive issues can also be a concern, and providers should be alert to the symptom of headaches as a potential marker of elevated blood pressure. Although rehabilitation professionals should routinely measure blood pressure in patients, numerous studies have demonstrated that we do not. The referenced guidelines give parameters for blood pressure readings for mild, moderate, and severely high blood pressure readings in pregnancy.
| High Blood Pressure in Pregnancy
|
Diastolic (mm Hg)
|
Systolic (mm Hg) |
| Mild | 90-99 | 140-149 |
| Moderate | 100-109 | 150-159 |
| Severe | ≥110 | ≥160 |
The third trimester and the postpartum period bring the highest risk for stroke, and the authors of the guidelines point out that a stroke can occur with even moderately elevated blood pressure readings. Even if a woman recovers from elevated blood pressure in the peripartum period, she may remain at risk for developing further cardiovascular disease including stroke. Having gestational diabetes, which can later develop into Type 2 diabetes, can also increase stroke risk, meaning that every woman's history related to pregnancy and postpartum cardiovascular health should be taken with interest. Measuring blood pressure regularly is also a habit that therapists must develop.
In addition to screening for elevated blood pressure in the peripartum period, rehabilitation providers can educate women in healthy lifestyle choices, safe exercise activities, and in management of musculoskeletal disorders that may inhibit physical activity. If you are interested in learning more about caring for women in the peripartum period, look ahead at dates for the continuing education course Care of the Pregnant Patient or Care of the Postpartum Patient
A recent on-line, national survey completed in Australia asked women who had completed treatment for breast cancer to answer questions about exercise. 432 women were surveyed about their perceived exercise barriers as well as potential benefits. Although the answers may not be entirely surprising to practitioners who work with women who are participating in cancer rehabilitation, we may be able to learn about ways to support women who are interested in increasing their exercise activities. Women reported challenges of feeling weak, lacking self-discipline, and not making exercise a priority as barriers to exercising. Women also reported enjoying exercising, having improved sense of well-being, and decreased tension and stress when participating in exercise. The authors in this study describe the potential physical benefits of exercise in survivors of breast cancer to include improved cardiorespiratory fitness, strength, energy levels, more effective weight management, and decrease in risk of heart and circulatory disease. Further benefits towards emotional and psychological health are also described in the study and include improved self-esteem, decreased anxiety and depression, and better mood.
With all of these known benefits, what limits exercise participation in women? Consider that a woman who is already dealing with cancer-related fatigue has a small reserve of extra energy. If she participates in exercise, will she have enough energy to prepare healthy foods, or to finish her work, or to interact with her family? Even though the exercises may in the long run increase a woman's energy levels, understanding the choices that she has to make on any given day can help guide the therapist's recommendations. How can you help a patient avoid procrastination, one of the largest perceived barriers to exercise in this study? Perhaps you can help her trouble-shoot the obstacles that she may face in her day and give examples of actions that can set her up for success. These strategies might include preparing her exercise clothing to bring with her for a lunch time walk, or taking a nap at work so that she has enough energy to exercise in the evenings. Engaging a friend to join her for exercise activities or helping her find a comfortable bra- one of the commonly mentioned barriers in the referenced study- may help a woman participate in exercise.
Many pelvic rehabilitation providers are working with women who are dealing with the challenging recovery associated with oncology issues such as breast cancer. Although women may know that exercise is beneficial, the barriers to exercise can limit participation in lifelong healthy habits such as daily exercise. Regardless of the type of cancer a woman is woman is recovering from, being able to dialog about perceived barriers to exercise is valuable. If you are interested in working with more women who are recovering from cancer, or in general would like to know more about exercise and oncology issues, the Institute has an oncology series with topics in breast cancer and pelvic cancer, among others.
In patients who failed to respond to biofeedback therapy alone for anismus, authors in this study reported a beneficial, although temporary, effect of using botulinum toxin type A injection (BTX-A injection) to the puborectalis and external sphincter muscles. Anismus is more commonly referred to as dyssynergic defecation, or an inability to properly lengthen the pelvic floor muscles during emptying of the bowels. 31 patients who had been treated with and failed "simple biofeedback training" were then treated with BTX-A injection followed by biofeedback training. 18 males and 13 females with a mean age of 50 and a mean duration of constipation of 5.6 years were diagnosed with defecation dysfunction, or anismus. Diagnosis of animus was made using anorectal manometry, balloon expulsion test, surface electromyography (EMG) of the pelvic floor, and defecography.
Pelvic floor muscle training included biofeedback therapy consisting of intra-anal surface EMG and electrotherapy (although the way the methods are described make determining if both EMG and electrotherapy were completed with internal sensors difficult). Treatment occurred 1-2 times/day for 30 minutes per session (15 minutes of electrotherapy and 15 minutes of biofeedback). Frequency of the electrotherapy was 10 Mz, 10 seconds of "considerable sensation without…pain" and 10 seconds of rest. During biofeedback sessions, pelvic muscle strengthening and relaxation was also instructed. Therapy occurred for up to one month, and patients were instructed to continue with therapeutic exercises at home. The researchers followed up one month after the injection and therapy, and 6-12 months after intervention by telephone.
The subjects in this study suffered from difficult and incomplete evacuation, use of laxatives, and chronic straining during defecation. The repeated measures for diagnostic criteria that were completed after intervention found improvements in the subjects' resting anal canal pressures and with the balloon expulsion test and constipation scoring system. The authors also reported adverse effects of BTX-A injections including fecal incontinence. Conclusions of the article include that the botox injections were considered a temporary treatment for defecation dysfunction, whereas the botox injection combined with pelvic floor biofeedback training is "a more valid way to treat."
What is missing from this study? Manual therapy, muscle coordination retraining in combination with abdominal wall activation, and functional training related to positioning. While the authors suggest that injections should be used with biofeedback training, the potential negative effects of botox injections cannot be overlooked. Infection, pain, and bleeding are complications that have been highlighted in the literature, and in this study, fecal incontinence (although reported as mild) occurred. The research design appears to fail to recognize the chronic tension and holding pattern of the pelvic floor muscles, and unless the goal of repeated contractions is to elicit a contract/relax effect, the pelvic floor strengthening per se does not align with the ideal therapeutic goal, which should be to correct the dyssynergic pattern of defecation. Relaxing the pelvic floor muscles is not the same as a functional bearing down or lengthening of the pelvic floor involved in defecation. If you are interested in learning more about training defecation patterns and pelvic muscle rehabilitation for bowel dysfunction, check out Pelvic Floor Level 2A (PF2A) which discusses in detail fecal incontinence, constipation, and other colorectal conditions. The next opportunity to take this course is in Wisconsin in March. If you have already taken PF2A, you might find a course focused on Bowel Pathology, Function, Dysfunction & the Pelvic Floor, with the next course taking place in Kansas City in April.
Pelvic rehabilitation therapists working with men who have sexual dysfunction may be aware of the work of Grace Dorey, who published a randomized, controlled trial about pelvic muscle strengthening for erectile dysfunction. A recent article published in the Journal of the American Physical Therapy Association confirms the conclusion of Dorey and colleagues that pelvic muscle rehabilitation is beneficial in improving erectile dysfunction.
In the study out of France by Lavosier and colleagues, 122 men with erectile dysfunction and 108 men with premature ejaculation completed twenty 30-minute sessions of pelvic muscle strengthening with active contraction and electrical stimulation. In the study, a penile cuff placed around the shaft of the penis measured intracavernous pressure, electrodes applied to the "upper face of the penis shaft" provided electrostimulation at 80 Hz to the ischiocavernosus muscles, and a vibrator device applied to the glans penis provided stimulation for erection. A large computer screen displayed contractions, and the patient was allowed to increase the level of electrotherapy stimulation to maximal sensory stimulation below pain threshold. Contractions were completed at the patient's own pace in regards to frequency and duration, but each patient did have feedback about his contraction on the computer monitor in front of him. Patients were also given an intracavernosal injection aimed to create an erection lasting 30 minutes.
The authors describe the erection process as being both vascular and muscular, with the ischiocavernosus muscle having a significant role in erections and in ejaculation. The ischiocavernosus muscle, which is a muscle of the superficial layer in the perineum, attaches along the ischiopubic ramus and wraps around the proximal superior portion of the penis to have an effect on penile rigidity. Contractions of the ischiocavernosus appear to maintain the rigidity of the penis through compression of the roots of the corpus cavernosum, the upper portions of the penis where blood fills in the spaces.
This is a very interesting study with equipment and software created specifically for the study. Because ischiocavernosus muscle force could not be directly obtained, force variations were measured using intracavernosal pressure changes during and after pelvic muscle contractions. The authors provide a detailed description of the analysis methods as well as the challenges of measuring the ischiocavernosus muscle with other methods. The lack of uniformity in the contractions and the likelihood that all components (pharmacological, electrotherapy, vibratory stimulation, and feedback) would not be a form of therapy available to all patients in a rehabilitation setting make this study challenging to extrapolate to patient care. However, further evidence that pelvic muscle strengthening can alleviate erectile dysfunction is promising, and the study components also bring into question if patients should be utilizing vibratory therapy, performing home exercise programs for longer periods of time (up to 30 minutes), and if patients should be completing their exercises during states of penile erections. Further research will help us understand the role of each component in pelvic rehabilitation and perhaps to also learn why the results of the study were not as encouraging for premature ejaculation.
To learn more about male sexual health and pelvic floor rehabilitation, you can attend the Male Pelvic Floor Function, Dysfunction, and Treatment continuing education course, with the next opportunity scheduled in Nashville in March.

Incontinence-associated dermatitis causes a range of signs and symptoms, and yet the potential impact of skin breakdown may lead to serious, even life-threatening consequences. Although patients of any functional status or within any treatment setting may be at risk for developing the condition. An article from Beeckman et al. in the British Journal of Nursing describes both the chemical and physical irritation of the skin that occurs when urine or feces remains in contact with the perineal skin. According to this article, urine and feces can cause an increase in the pH levels, and subsequently increase skin permeability, reduce barrier function, and increase the risk of bacterial colonization. Rubbing of the skin on clothing, pads or diapers, or surfaces such as a bed or chair creates friction and can further irritate the skin. The linked article focuses on the differentiation between incontinence-associated dermatitis (AID) and pressure ulcers, and is available for free, full access via the link above if you are interested in learning more about the concept.
If the skin dysfunction is limited to IAD, the pelvic rehabilitation provider may observe rash and erythema with possible skin breakdown, or infections such as candidiasis. Unless a therapist is trained in assessing for pressure ulcers, any new or worsened skin breakdown should be brought to the attention of a physician, nurse, or physician extender who is working with the patient. One of the challenges in perineal skin irritation is that the patient may not be able to easily observe the skin and report new onset or worsening of symptoms. In an outpatient setting, even when working with patients who do not have limited mobility or self-care skills, observing the perineal skin remains critical in documenting skin integrity, persistent issues, or a worsening of a condition. Because, as the authors of this study point out, care for skin ulcers and incontinence-associated dermatitis are different, early recognition and proper diagnosis aids in healing.
Following are some recommendations by Beeckman and colleagues for avoiding skin irritation in the presence of incontinence:
•A perineal cleanser should be used that has a pH range of 5.4-5.9
•Perineal skin should be cleaned quickly following an episode of fecal incontinence, whereas avoiding too-frequent skin washing with continual episodes of urinary incontinence is important
•Moisturizing the skin (with emolient-based rather than humectant-based moisturizer) is valuable in aiding healing and preventing further irritation
•Use a skin protectant to create a barrier between the skin and feces or urine
•Absorptive or containment products (catheter or stool diversion system) can further help keep irritants away from the skin surface
Ideally, issues of incontinence, topics covered at length in the Institute's introductory pelvic floor course series are treatable. Even in the case of refractory incontinence, patients should be made aware of appropriate treatment options and screening by appropriate medical providers can direct patients to proper diagnostic testing and referrals. Because pelvic rehabilitation providers may be the first to notice skin breakdown or risk for infections, recognizing our role in patient education and referral to proper providers remains essential.

From time to time, pelvic rehabilitation therapists ask this question: Does a pelvic rehabilitation therapist really need to "go there?" In other words, is subjective history taking, or perhaps surface electromyography (sEMG) enough of an evaluation and intervention to provide adequate care to patients with pelvic dysfunction? The short answer is no, and here's why: surface EMG is ONE tool for examination and intervention, and one that has limitations. The benefits of using sEMG are numerous: biofeedback has been utilized in much of the pelvic rehabilitation literature, with demonstration of efficacy as an intervention in conditions such as pelvic pain, incontinence, pelvic floor muscle training, and strengthening. Surface EMG, once equipment is acquired, is a relatively inexpensive method for providing feedback, or information about a typically unconscious activity, to the patient. Ideally, the patient internalizes the learned skills based on the biofeedback training and that skill is translated into functional applications such as letting go of a muscle group to avoid tension and pain, or activating a muscle to provide stabilization or protective contractions. So why is biofeedback alone not such a great approach?
Biofeedback does not always provide accurate information about a state of muscle contractility. Consider this fact which was highlighted effectively in Fitzgerald and Kotarinos' 2-part article about the "short pelvic floor": muscles need to produce an electrical event through firing of the motor units (action potential) in order to generate a reading on the biofeedback. When a muscle is in a contracture, or shortening without an active holding of the muscles, surface EMG readings can look "normal" even in the presence of tense, short, symptom-producing pelvic floor muscle states. Unless a therapist is using pressure biofeedback, inaccurate information is then provided to the therapist. Why else would a biofeedback-only approach not provide needed data upon which a pelvic rehabilitation provider bases his or her plan of care? Simply placing external sensors on the perineum or having a patient insert an internal sensor (without therapist observation or placement of the sensor) does not allow for appropriate inspection of the perineal skin, for the presence of prolapse, for the assessment of muscular tension or identification of tissues that are dense, tense, or pain-producing.
If sEMG is utilized in place of perineal observation, internal assessment, or interventions such as therapeutic activity, the therapist misses out on the opportunity to determine muscle tone, muscle tenderness in hard-to-reach places like the obturator internus muscle belly, or the nerve branches near Alcock's canal. It is impossible to know if one side of the pelvic floor is overactive, while the other side is non-functioning due to an old nerve injury or a new onset nerve dysfunction, if the sensors are testing both sides of the pelvic floor simultaneously. And finally, the lack of palpation and proper diagnosis can perpetuate a disconnect for the patient who is potentially relying upon external input rather than tuning in to her own body through the palpation, proprioception, and feedback of muscle states that the therapist can influence by using other evaluation and intervention skills. Consider also the challenge of keeping patients tethered to an sEMG device while trying to perform functional activities such as a golf swing, a lunge, or a jumping maneuver.
In my experience that includes teaching and mentoring of many students and therapists, it has been my observation that when therapists are a bit shy about their internal evaluation skills, sEMG may be relied upon too heavily. External (or internal) sEMG should not be the basis for a pelvic floor muscle training program for every patient. Of course, there are instances when a patient is not a candidate for internal pelvic muscle examination, and sEMG can be a terrific external option. Every patient who presents with indications for, and who does not present with contraindications to a pelvic floor muscle evaluation, should be provided with appropriate internal evaluation and intervention skills, rather than an external-only, sEMG-only approach. A therapist's toolbox should include a multitude of methods with which to approach each patient who presents with pelvic dysfunction.

Can palpation of the coccyx provide an objective screening tool to assess appropriate identification of pelvic floor muscles in patients? Researchers in the UK aimed to determine if external palpation of the coccyx bone would allow an examiner to evaluate pelvic floor muscle activity in women for functions of pelvic muscle contraction or bearing down/straining. Because the pelvic floor muscles, in particular the levator ani muscles, attach to the coccyx via thickened connective tissue, an effective lifting contraction of the pelvic floor muscles should create a flexion movement in a healthy coccyx or tailbone. Likewise, a bearing down may produce an extension movement of the coccyx palpable to a finger placed over the bony landmark.
In this study, 24 healthy women (whom the researchers knew could appropriately contract their pelvic floor muscles) volunteered to participate. The median age of the participants was 57 years old. Results of the study include that the researchers were able to correctly evaluate a contraction, bearing down, or resting position of the coccyx in 56/58 observed.The authors conclude that the coccygeal movement test, or CMT, can be a useful screening test for determining if a woman can appropriately locate and contract the pelvic floor muscles, or PFM. The CMT can be performed in a sitting position or with the subject in a side lying position. In the research study, subjects wore light clothing and were assessed in sitting. The tester placed the middle finger on or close to the coccyx. A correct contraction was considered one in which the coccyx flexed or moved inward. (The participant chose a notecard with the requested action- contract, relax, or neutral- that were shuffled, so that the investigator was blinded to the movement the subject would be completing during the assessment.)
The results of the study indicated that the coccygeal movement test was sensitive (could predict if the woman correctly located her pelvic floor muscles), but not specific (some of the women who could in fact locate the PFM were identified as not being able to locate them.) The authors do not suggest that this external screening test should replace vaginal palpation in women who may require pelvic floor muscle training. Rather, they offer that this simple, non-invasive screening test may provide a method for confirmation of a correct contraction in situations when women are instructed in preventive pelvic floor exercises, such as during prenatal visits. Because many women who are instructed to complete pelvic floor exercises are not offered objective confirmation of appropriate contractions, this test may serve as a middle ground for providers in environments when a quick screen is most appropriate. The authors do caution that the test may misidentify a woman as not being able to properly contract when in fact she is able to contract.
Examination and treatment skills for coccyx are included at length in the course Pelvic Floor Level 2A, in which both external and internal treatment skills are acquired. The next PF2A course is filling up quickly for its scheduled event in Wisconsin in March of next year. The Coccyx Pain: Evaluation & Treatment continuing education course created by faculty member Lila Abbate is back in 2015, a course entirely based on coccyx dysfunction and rehabilitation. The next opportunity to take Lila's course is in California in March.

A recent case report in the Journal of Physical Therapy Science describes the benefits of specific strengthening of the subdivisions of the gluteus medius in a patient with sacroiliac joint pain (SIJ). The intervention is based in prior research that demonstrated varied muscle firing patterns in the gluteus medius during different exercises. The author of the study suggests that the stabilizing role of the gluteus medius can influence sacroiliac joint pain.
The patient in the case report was a 32 year-old female who complained of pain in the left iliac crest area and sacroiliac joints for 6 months. Symptoms worsened with forward bending, standing for more than an hour or walking for more than thirty minutes. Before and after a 3 week intervention of specific strengthening exercises, objective tests included the Gaenslen, Patrick, and the resistive abduction (REAB) test. These tests were all positive for pain provocation. Exercises were instructed for gluteus medius strengthening and were performed over a period of three weeks. Following the 3 week exercise intervention focused on gluteus medius strengthening, the patient's Visual Analog Scale improved from a 7/10 to a 3/10, and repeated objective tests were negative. Exercises for the various portions of the gluteus medius (GM) were prescribed at 3 sets of 30 repetitions/day and are as below:
Keeping in mind that this case represents only one clinician/patient interaction, we can ask ourselves several questions about the positive results of the intervention. Are we currently challenging the hip abductors enough with our patients who have pelvic girdle pain, and is there enough specificity in the exercises to challenge the appropriate muscle fibers? Can isolated strengthening of hip abductors in absence of other interventions have a positive effect on sacroiliac joint pain in our patients? Are there other plausible rehabilitation concepts inherent in performing these open and closed chain activities that contributed to improvement in this particular patient, rather than an isolated increase in muscle training for the gluteus medius? The sacroiliac joint can be a confounding source of pain, and at the same time, successes in treating patients who have SIJ dysfunction can be very rewarding. If you would like to learn more about evaluation and treatment of sacroiliac dysfunction, the next opportunity to take faculty member Peter Philip's course Sacroiliac Joint & Pelvic Ring Dysfunction, offered next in Seattle in January.
This post was written by H&W instructor Ginger Garner. Ginger will be presenting her Hip Labrum Injuries course in Houston in 2015!

There are two accepted forms of hip impingement currently documented in the literature. The two types are 1) CAM type FAI (femoracetabular impingement) and 2) Pincer type FAI. These two types are found inside the joint, meaning they are considered intra-articular bony anomalies.
FAI is a common comorbidity found with hip labral injury (HLI); and in fact, FAI is a risk factor for HLI. Specifically, FAI is a bony impingement that arises in the femoral head-neck function and the rim of the acetabulum (see photo at right). The two types of FAI also generally occur together more than they do in isolation. However, it is possible that, combined with other issues like acetabular undercoverage or hip instability, CAM or Pincer-type FAI can be found a singular diagnosis.
Surgical Intervention
However, the arena of impingement in the hip is now evolving to consider other locations. In the past 5 years there has been buzz about other types of FAI. They aren’t classically considered FAI issues since this new type of identified impingement occurs outside (extra-articular) the joint. One type newly identified is known as anterior inferior iliac spine/subspinal hip impingement (AIIS). In a 2011 study of 3 case reports, AIIS was found and treated with arthroscopic AIIS decompression with positive results. A more recent 2012 study found excellent results at short-term follow up for surgical decompression of AIIS.
Identification & Diagnosis of AIIS
Both personal and professional experience in the area of AIIS has shown that AIIS is not always discovered on an AP (anterior-posterior) radiograph. However, it is possible to see a larger AIIS on an AP film. Another helpful (but not always definitive) diagnostic test is a CT scan with MRI 3D reconstruction (and no contrast). Bony contrast is more reliable with CT scan than the typically preferred MRA (which is better for soft tissue contrast).
In addition, the rectus femoris (RF) could be implicated in AIIS pathology because the same area receives the proximal attachment of the RF. The same 2011 study reported that the morphology and role of the RF in extra-articular impingement is “not well reported at this time.”
Likewise, the identification of AIIS as a primary driver of pathology in intra-articular hip injury (FAI and/or HLI) is rare. Some cases of AIIS are being found during hip arthroscopy to correct identified existing deficits such as FAI and/or HLI. This means that AIIS may be missed and should be included as a potential mechanism of injury, especially for anterosuperior labral tears in the 2 to 3 o’clock region.
Patients who have AIIS may present like a typical HLI patient, which means they may have a positive Thomas test, FADDIR test, or mechanical symptoms such as popping, clicking, grinding or giving way. It is important to note these signs and symptoms and work in a team approach with surgeons and physical therapists who specialize in hip preservation and reconstruction.
To learn more about nonoperative and operative hip labral and FAI management, check out faculty member Ginger Garner's continuing education course on Extra-Articular Pelvic and Hip Labrum Injury: Differential Diagnosis and Integrative Management. The next opportunity to take the course is March of 2015 in Houston.
According to the World Health Organization (WHO) sexual health relies upon a "…positive and respectful approach to sexuality and sexual relationships, as well as the possibility of having pleasurable and safe sexual experiences, free of coercion, discrimination and violence." This definition provides an excellent framework, yet how many of us were provided with the tools we needed growing up to understand the many domains that affect sexual health such as physical (how does sex work?), and social and psychological implications? Herman & Wallace Pelvic Rehabilitation Institute co-founder Holly Herman has been a long-time proponent of sexual health and function, and in courses, she might be heard asking participants to consider most individuals first sexual encounter: was it relaxed, were both parties informed, was the experience pleasurable? Regardless of a person's stance on when an individual should first engage in sexual activity and with whom, developing a life-long healthful approach to our own sexuality is clearly an integral part of optimizing quality of life.
Ff we expand this concept to the pelvic rehabilitation caseload we often face, how can we best meet the needs of our patients if our own education in sexuality was limited? How can we best understand the varied approaches to sexual health and function if the approaches do not match our own? Our world has fortunately shifted to include the recommendation that healthy sexuality begins in childhood. The American Academy of Pediatrics states that a simple step in childhood sexual development is in using the correct anatomical names for genitalia. How can youth and adolescent sexual health education and support be improved to further promote lifelong healthy sexuality?
An article published last year in the journal Public Health Reports addresses a paradigm shift from teenage pregnancy prevention to youth sexual health. The Oregon Youth Sexual Health Plan was developed in 2009 following a collaborative effort from state agencies and private partners, and focuses on "development of young people" and embracing "sexuality as a natural part of adolescent development." This article lends historical perspective to the advancement of the concept that adolescents have a right to sexual health knowledge, not simply in relation to reproduction and sexually transmitted disease, but also in relation to quality of life and interpersonal relations. The researchers also point out the failure of abstinence-only sex education to produce significant evidence of efficacy.
Goals of the youth sexual health plan include having young people use "accurate information and well-developed skills to make thoughtful choices about relationships and sexual health." Additional goals include that sexual health inequities are removed, rates of teenage pregnancy and sexually transmitted diseases are reduced, and non-consensual sexual behaviors are reduced. The Oregon Youth Sexual Health Plan is public policy, and one that may pave the road for other states seeking to move from a negative stance that focuses on potentially harmful impacts of sexuality to a positive sharing of needed information, knowledge, skills, and support in developing a healthy view of sexuality. If you would like to learn more about sexual health and sexual medicine, join Holly Herman at her course titled Sexual Medicine for Men and Women. The next opportunity to take this course is in January in Houston!
By accepting you will be accessing a service provided by a third-party external to https://hermanwallace.com./